Anniversaries and Obamacare
Today is the one-year anniversary of the big surgery: 78-pound, five-foot-tall “M’, 87 years old and a feisty New York native, was operated on for tongue cancer. The surgery meant removal of half her tongue followed by its reconstruction using the long muscle of her forearm. It included removing all the lower teeth on one side and a long incision with careful dissection of the muscles of her neck. The operation included a skin graft from her thigh to cover her arm wound.
M was in the operating room over 10 hours and relied on the skills of three surgeons: aged 71 (her gifted ear, nose and throat doctor), 65 (her plastic surgeon) and 58 (the youngster, her oral surgeon). Three surgical fellows and residents and two medical students observed. Half a dozen nurses rotated in and out. And M survived.
Her story began seven years earlier when a non-healing tongue ulcer proved to be a squamous cell cancer. As a life-long nonsmoker and non-drinker, M wracked her brain trying to figure out the cause. No papilloma virus. No exposure to toxins. Nothing but dumb, bad luck. So the tongue lesion was removed leaving her with thick speech. Six months of radiation therapy followed and she was good to go.
You see, M wanted to live and would do anything the doctors suggested. She was otherwise healthy. A widow with young grandchildren, she had birthdays and graduations to enjoy and holidays to cook for. She lived for her family. She had been raised by a single father in a New York City apartment with two older sisters (her mother died when M was three, succumbing to tuberculosis). They were second-generation Italians thankful for the 5th floor walkup and the opportunities the city provided.
M finished high school and worked during WWII in her dad’s shop. She became an artist and worked in oils and made prints. She married the handsome naval officer from the neighborhood, even though he was from the Irish side of the street. They moved to “the Island” (Long Island) and raised a son, while M pursued joy in her landscape painting.
M was a giving mother, doting grandmother and a good American. She volunteered at church, taught art at the local Catholic schools, and took care of herself and her family. She paid her taxes and encouraged her son to give back to others and supported him through his graduate school training. But one year ago today, at age 87, a healthy seven years after radiation treatment, she was losing weight and facing the dreaded cancer diagnosis once more.
This time, however, there was no quick fix. She was seven years older and despite being independent, living alone and caring for herself and her own home, she was weak from weight loss. She appeared frail. The surgeons gave her a 50-50 chance of surviving the surgery…and if she did, there would be months of rehab and possibly permanent disability in being unable to talk or feed herself. She would need a feeding tube to her stomach indefinitely. And she could have a stroke or other catastrophic event in the post-operative period. The alternative was to make her comfortable….or, as President Obama has said, she could just take “the painkiller…” M’s family doctor was brutally frank about the difficult path ahead.
The crux of the matter is, M and her family had a choice. She was given the options and the non-sugarcoated reality of the tough road of surgery. The surgeons spent time with her and noted her indomitable spirit and her supportive family. They had years of experience with cancers like hers and the patients who had survived them. And working with patients like her allowed them to teach the younger doctors the techniques and skills that enabled them to help patients with such advanced cancers. The doctors had options and could exercise them. The patient also had options. They worked together and devised M’s treatment.
The surgery went as well as one could have hoped. The next three weeks were difficult, with an episode of heart failure and unrelenting diarrhea. M was frustrated that she couldn’t talk and even more upset that others had to care for her. But she persevered, and by day 24 was discharged to her son and family. Six months later, she was back in her own home: talking, cooking, ordering Harry and David fruit baskets for the therapists who had helped her along, and teaching in her art group.
M made another round of Thanksgiving, Christmas, and Easter, birthdays, a grandchild’s musical performance, and a granddaughter’s high school graduation. Despite the long haul, when asked, she said she would “Absolutely!” go through it all again. “I would never have missed all this!” “This” i.e., life.
So what would have happened differently to M under the Affordable Care Act, i.e., Obamacare, had it been in place when she found her cancer had recurred? Would her visit to the ENT doctor have occurred in a timely fashion? Would her surgery have been approved? Would the patient review panels approve a $100,000-plus surgery and hospital time for an 87-year-old widow? Hadn’t she had enough life? Would it have been fair to allot limited resources to one so old with such a limited lifespan when those medical dollars could have gone elsewhere, say, to better preventive health programs? Shouldn’t she have been handed a painkiller and told to take it, for the good of her country and her family, and not be a burden? Would her doctors have even been permitted to discuss a surgical option with her at all?
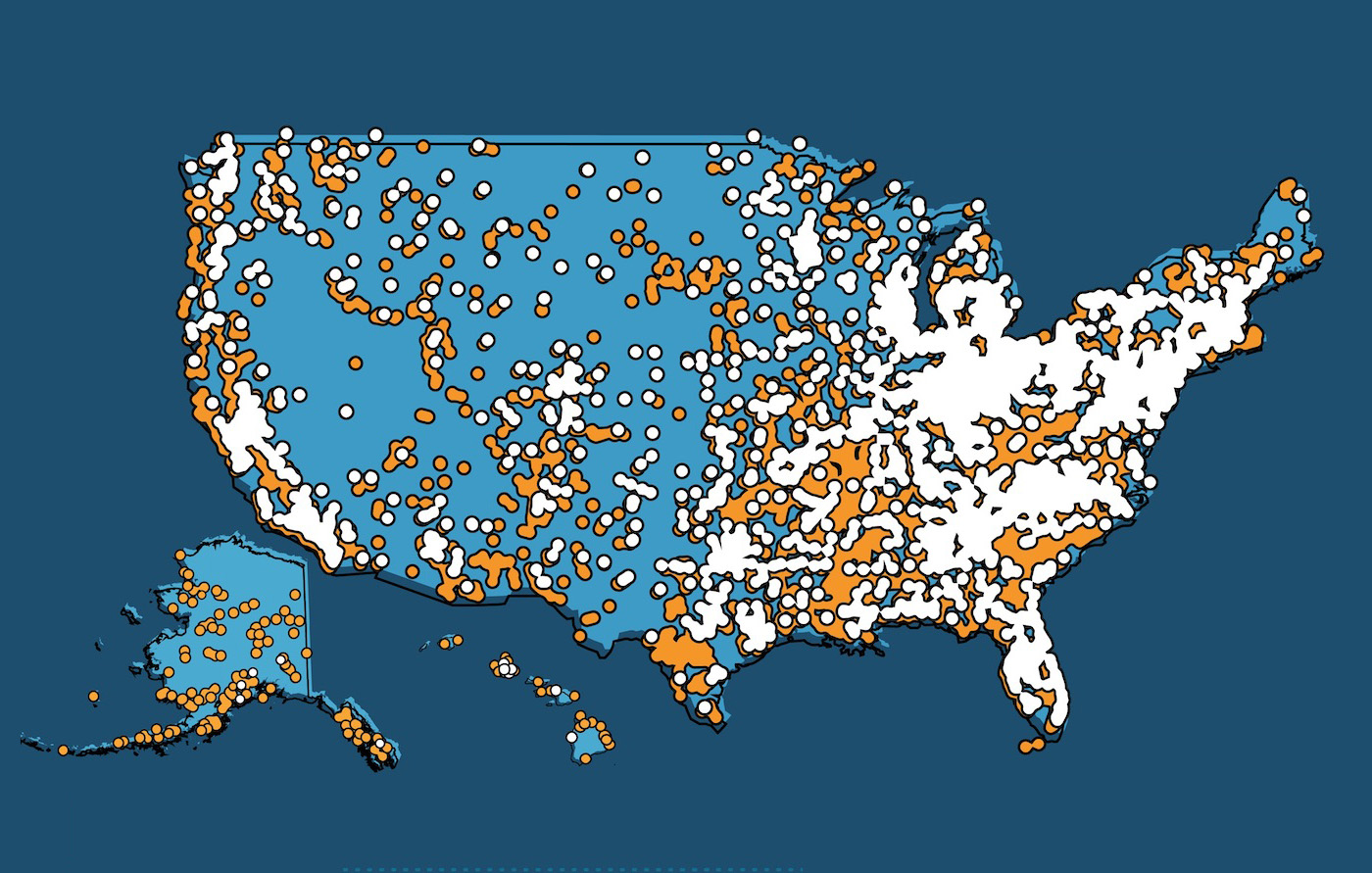
M is one of the 500,000 Medicare patients in Connecticut and one of the 15% of those patients in Medicare Advantage. Under the new Affordable Health Care Act, her insurance with United Health Care is no longer available. She doesn’t know yet if her surgeons have been dropped. Two of her surgeons have said they will retire rather than deal with the hassles of the new regulations. She does not know if ENT coverage for a cancer of her type is covered. If it is, what limitations on surgical intervention and adjuvant therapies are in place?
M needs an advisor with plenty of time and expertise with medical billing and coding to guide her forward…unlike last year, when her family doctor could talk with her and then pick up the phone and refer her to the best doctor with the most experience. Now even primary care physicians are retiring or being forced out of Medicare Advantage. In New York state, 8,000 seniors on Medicare Advantage have just learned that their doctors are dropped from the plans. Like them, M’s care may begin anew with a “health care provider’ who may have no incentive to know or interest in knowing how best to care for the feisty lady from New York. To him or her, she may just be another elderly lady to keep comfortable…
Geriatric care in this county has been improving for decades. The average 80 year old can see his lifespan increased another 10-15 years with advances in cardiac care, cancer therapy, and infectious disease antimicrobials. A primary care physician could build a rapport with the patient, and, together, they could responsibly make decisions on aggressive therapies and end of life care.
But with the Affordable Care Act, with its laudable goals of providing care for the indigent and access for everyone, doctors and patients are losing. Primary care physicians are asked to see too many patients for less and less remuneration. Thirty million previously uninsured Americans are being “guaranteed” access to these physicians while medical schools and residency programs are producing fewer internists and family doctors every year.
In fact, a soon-to-be released study by the Association of American Medical Colleges discussing the role of medical schools’ culture in primary career choice by Erikson et al. appears in the December, 2013 issue of the AAMC‘s journal Academic Medicine. The authors surveyed all 4th-year medical students from a random sample of 20 medical schools to assess both student and school-level characteristics that were associated with greater likelihood of entering primary care.
The first and arguably most important finding was that only 13% of these final-year students were planning on primary care careers, despite the fact that 40% had originally planned to do so when admitted to medical school. Once the students were exposed to the uncertainties of primary care, both financially and professionally, they opted for other fields.
Moreover, older physicians, those with the judgment and experience, are retiring in record numbers. Deloitte’s 2013 survey of U.S. physicians found that 57% of doctors view changes in the industry under the Affordable Care Act as a threat, and six in 10 physicians report it is likely that many will retire earlier than planned in the next two to three years. This trend could cause more widespread issues in a health-care system that is already coping with doctor and nurse shortages in some areas of the country.
And doctors are not alone in being adversely affected. Hospitals are being graded on how quickly Medicare patients are treated and discharged, and penalized if the patients rebound (i.e., are readmitted) too quickly. The incentives now lie in volume and dotting every ”i” on mountains of paperwork, while the patient, with his or her story of growing up hardscrabble in New York City and only wanting to make it to Christmas, is being ignored.
How many M’s out there won’t have that extra year of life because the numbers/the rationers/the administrators decide against her? Yes, there are many, many problems with health insurance and runaway costs in the United States, but the regulations of Obamacare have only made a challenging situation more difficult.
For the sake of all the M’s out there and the physicians who care for them, the Act needs to be scrapped and the business of health care needs to be readdressed – this time, with doctors and patients sharing the responsibilities and solutions.
Keiren D. Smith, M.D. is an associate scholar of the Charlotte Lozier Institute.