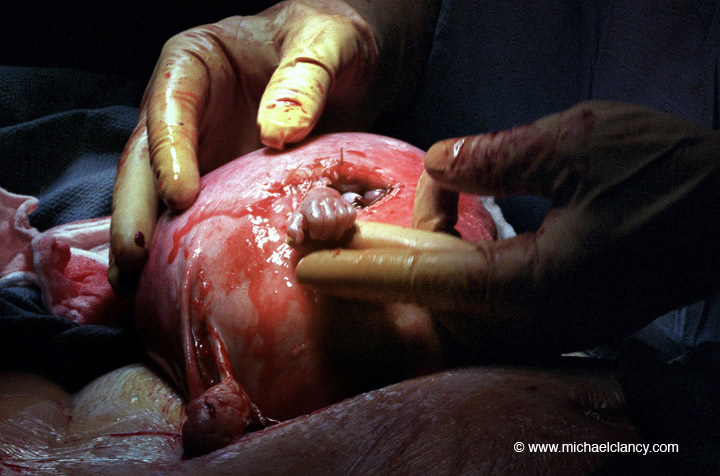
Parents may receive news during routine ultrasound scans and testing that their baby or babies have a disease, disorder, or structural defect. But there is hope. Recent medical and surgical advances have made it possible for some babies to receive life-saving treatment while still inside the womb—long before they are even born!
Become A Defender of Life
Your donation helps us continue to provide world-class research in defense of life.
DONATECharlotte Lozier Institute
Phone: 202-223-8073
Fax: 571-312-0544
2776 S. Arlington Mill Dr.
#803
Arlington, VA 22206
Fetal Surgery: Treating Babies Before They are Born
Parents may receive a prenatal diagnosis of spina bifida, a severe disorder in which part of the baby’s spinal cord does not close properly. Depending on the location of the damage, spina bifida can cause neurologic and intellectual impairment, including paralysis. While surgery in the first few days after birth can help, doctors have discovered that performing revolutionary surgery to repair the baby’s defect before birth, while still in the mother’s womb, leads to better outcomes for the child.1 In a groundbreaking study published in the New England Journal of Medicine, treatment of babies in the womb was so successful that the trial was stopped early, so that treatment was not withheld from babies randomly selected to receive standard postnatal repair. The study found that when fetal surgery was performed on fetuses before 26 weeks, there was a decreased risk of death or shunting before the age of one, as well as improved mental and motor function (including independent walking) at 30 months of age.2
Other parents may receive a prenatal diagnosis of twin-to-twin transfusion syndrome (TTTS), a serious and life-threatening condition for both babies caused by abnormal connections in blood flow between identical twins who share one placenta. This leads to an imbalance in blood flow in which the smaller (donor) twin pumps blood to the other, larger (recipient) twin. If left untreated, advanced forms of the disease can be fatal. This minimally invasive surgery, called fetoscopic laser ablation, uses small, fiber-optic guided instruments called endoscopes to create one small incision to disconnect the shared blood vessels in the placenta between the connecting twins. If performed promptly, fetoscopic laser surgery is the best option for saving both babies, particularly when the disease is identified in its early stages. High volume fetal therapy centers report a higher than 90% survival rate of at least one baby and a higher than 80% survival rate of both babies after fetal surgery to correct the defect.3
Some surgeries have even been performed as early as 12 weeks gestation.4 More surgeries are performed by 15 weeks gestation,5 6 7 but the majority of prenatal surgeries occur after 20 weeks gestation.8
Fetal surgery has also proven successful in treating the unborn for several conditions including sacrococcygeal teratoma (SCT), congenital diaphragmatic hernia (CDH), congenital cystic adenomatoid malformations (CCAM), severe kidney obstruction and oligohydramnios, bladder obstruction, and others.10 This is not to mention all of the in utero therapies currently available to treat the unborn, such as maternal steroid therapy to promote lung maturity in premature fetuses and reduce respiratory distress syndrome (RDS).
Amidst the pain and despair of receiving a fetal diagnosis, fetal therapy and surgical interventions provide real hope to parents. It is now possible for fetuses with previously life-limiting or life-threatening diagnoses to not only survive to birth, but also to experience marked increases in quality of life and lifespan.