Letter from Aaron Kheriaty, M.D., to American Medical Association in Opposition to Physician-Assisted Suicide
For almost a quarter of a century, the American Medical Association (AMA) has opposed physician-assisted suicide, stating that it is “fundamentally incompatible with the physician’s role as healer, would be difficult or impossible to control, and would pose serious societal risks.” In strong language, the AMA has concluded that “permitting physicians to engage in assisted suicide would ultimately cause more harm than good” and that physicians “should not abandon a patient once it is determined that cure is impossible.”
This March and June at its Interim and Annual Meetings, respectively, the AMA will review its stance and consider whether it should reaffirm or amend its long-held opposition to assisted suicide. It is noteworthy that prior to California’s passage of legal assisted suicide last year, its state medical association rescinded its 28-year opposition and declared neutrality. As a part of the review process, AMA’s Council on Ethical and Judicial Affairs (CEJA) is collecting data, position statements, and relevant literature on assisted suicide during this time. The Charlotte Lozier Institute is especially grateful to Dr. Aaron Kheriaty, a clinical psychiatrist with expertise in suicide, for granting us permission to publish his November 2015 letter to the AMA CEJA on this critical issue.
To view this letter as a PDF, see here.
Dear Members of the AMA Council on Ethical and Judicial Affairs:
I am writing as a fellow physician to strongly encourage you, as well as the AMA House of Delegates, to maintain the AMA’s longstanding opposition to physician-assisted suicide. Among the many serious problems with permitting this practice I will mention just a few, which concern me not only as a physician and medical ethicist, but also as a clinical psychiatrist with expertise in the problem of suicide.
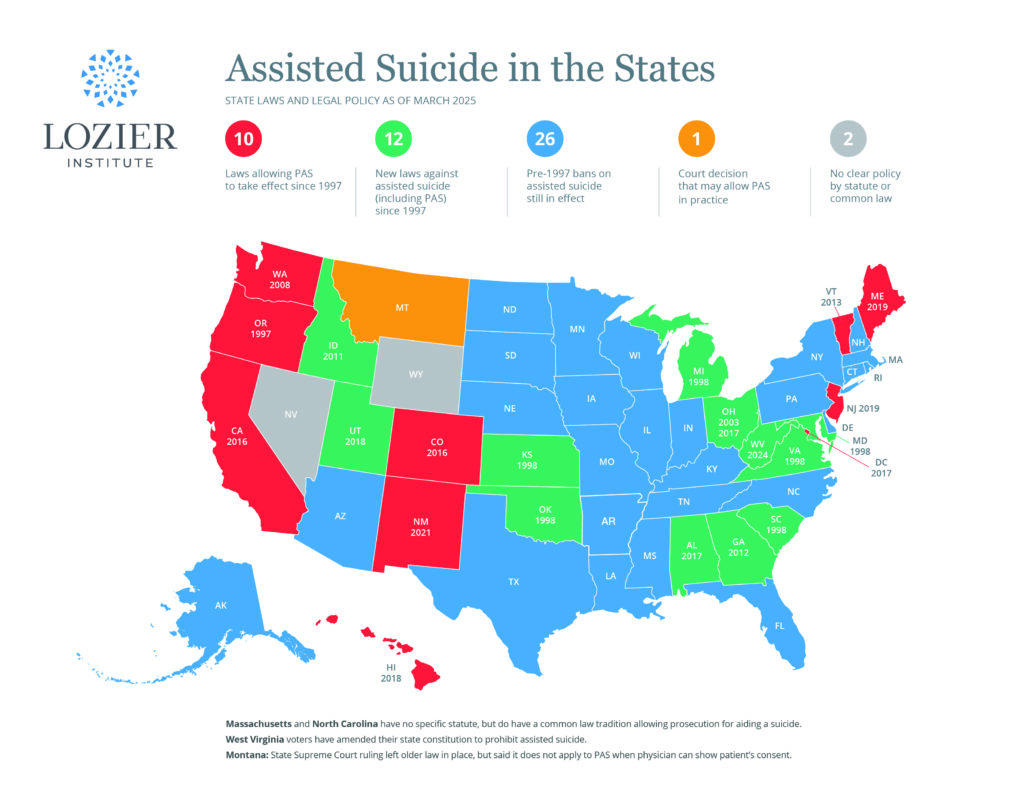
Current laws in the states that permit assisted suicide, including California, Oregon, Washington, and now Colorado, do not require physicians to refer for psychiatric consultation to rule-out the most common mental disorders or other causes that contribute to suicidal thinking and the wish to die. Many Americans already lack necessary access to mental health care services, and these laws places these and other vulnerable individuals at risk. The desire to end one’s life, or the request for assisted suicide, is nearly always a cry for help. It is a distress signal, a kind of “canary in the coal mine,” indicating that something in the patient’s situation (medical, psychological, or social) is not adequately being attended to – an untreated clinical depression, fear or anxiety about the future or about one’s medical condition, untreated or undertreated pain, family or relationship strain or conflict, and so on. Well-replicated research demonstrates that 80 – 90% of suicides are associated with clinical depression or other treatable mental disorders, including for individuals at the end-of-life and individuals with a terminal condition (cf. Admiral P., cited in: Lo B. Euthanasia: the continuing debate. West J Med. 1988;49:211-212). Yet alarmingly, according to the Oregon Health Department’s annual report, only 5% of the individuals who have died by assisted suicide under Oregon’s law were referred for psychiatric evaluation – and this number is decreasing every year. Considering what we know about suicide risk factors, this constitutes medical negligence.
This concern that the risk that serious mental health issues will be overlooked in the application of these laws is not merely theoretical: Consider the case of Michael Freeland, an Oregonian who had a 43-year history of depression and had made prior suicide attempts; and yet the physician who prescribed the deadly drug for him did not deem it necessary to refer for psychiatric evaluation or psychological counseling. While this is clearly negligent, there is nothing in the Oregon Law, or the current permissive laws in other states, to prevent this. The laws are in fact designed primarily to protect physicians, not patients: according to the newly enacted law in California, the physician is protected from all scrutiny and liability so long as he is acting “in good faith.” This minimal “good faith” legal standard is found nowhere else in medical practice, where physicians are required to practice according to the higher “medical standard of care.” The family of someone like Michael Freeland has no recourse as long as the physician claims he was simply acting in “good faith.”
The social consequences of suicide are significant and should not be ignored. Studies have repeatedly demonstrated a “social contagion” aspect to this behavior, which leads to copycat suicides—this is known by scientists as the “Werther Effect” in social science. The work of Nicholas Christakis and others have also demonstrated how suicide, like other health related behaviors, tends to spread person-to-person through social networks; the statistically significant influence extends up to three degrees of separation (Christakis, NA; Fowler, JH: Connected: The Surprising Power of Our Social Networks and How They Shape Our Lives. Little, Brown and Company, 2009). Indeed, it is noteworthy that the overall suicide rates in Oregon rose dramatically in the years following the legalization of physician assisted suicide in that state in 1997: after Oregon’s suicide rates had declined in the 1990s, they rose alarmingly between 2000 and 2010, surpassing the rate of increase nationally. Preliminary data from Washington shows a similar trend.
Of particular interest here is a study published last year by Jones and Paton, who analyzed the suicide data from Oregon and Washington. After controlling for other factors that could account for the rising rates of suicide in these states, their analysis suggested that there is indeed a causal link between the legalization of assisted suicide and an increasing in overall suicides in both states. This finding of a statistically significant increase in overall suicide rates, and an upward trend in unassisted suicide rates, undermining Posner’s hypothesis that legalizing assisted suicide would lower overall suicide rates. (Jones DA, Paton D. How Does Legalization of Physician-Assisted Suicide Affect Rates of Suicide? Southern Medical Journal. 2015 Oct;108(10):599- Cf. also Kheriaty, A. Social Contagion Effects of Physician-Assisted Suicide: Commentary on How Does Legalization of Physician-Assisted Suicide Affect Rates of Suicide? South Med J. 2015 Oct;108(10):605-6.) While more research needs to be done on this issue, the initial results here are cause for serious concern.
Laws have a pedagogical function; the law is a teacher, and these laws send the message that under difficult circumstances, some lives are not worth living. Unfortunately, this is a message that will be heard not only by terminally ill individuals, but by all vulnerable persons who are tempted to take their own lives. Suicide is now a public health crisis: according to the CDC suicide is currently the 2rd leading cause of death among adolescents and young adults, and the 10th leading cause of death overall for adults. We have evidence now that permitting physician-assisted suicide will worsen this public health crisis.
There are ethical issues of justice and equal protection as well. A law allowing assisted suicide for some individuals creates two cohorts of patients, who no longer enjoy equal protection under the law or equal medical care. Assisted suicide is discriminatory, and the basis for discrimination is the patient’s health status. Robin Williams walks into my office saying his life has become unbearable and so he wants to take his life; and I intervene to protect him and get him through the crisis. Then Brittany Maynard walks into my office saying her life has become (or will soon become) unbearable and so she wants to take her life; and not only do I not intervene to prevent her, but I actively engage in helping her to take her own life? These two incompatible approaches to suicide cannot co-exist side-by-side within medicine or mental health care—something will have to give. Laws that permit physicians to assist some patients in taking their own lives will undermine the medical and psychiatric community’s necessary efforts aimed at suicide prevention.
Supporters of permissive legislation on this issue generally constitute a homogenous elite: white, upper and middle class, well insured, well educated, able to navigate the complex healthcare system. These are precisely the folks least likely to be harmed by permissive laws. We don’t see widespread support from minority communities, from the uninsured or underinsured, from the economically or socially marginalized. What they want is access to good healthcare. They need Medicaid to pay for palliative care. They need hospitals in their communities not to close down.
In order to maintain the public trust in our profession, medicine must adhere to its foundational ethical principles. Our mandate must remain: when possible to cure, always to care, but never to kill. Physician assisted suicide is bad for medicine; it places vulnerable patients at risk, and ignores the real end-of-life healthcare issues for most Americans. I strongly urge you to consider these ethical and public health issues, and maintain the AMA’s position in opposition to this practice.
Aaron Kheriaty, M.D., is Associate Clinical Professor of Psychiatry at the University of California Irvine School of Medicine, where he also serves as Director of the Program in Medical Ethics.