Researchers Create First Human-Chicken Hybrid Embryos


Scientists at New York City’s Rockefeller University recently created the first human-chicken hybrid embryos and used them to identify the presence of a human developmental cell organizer; the creation of the hybrid embryos has caused some to question the ethical implications of grafting embryonic human cells into other species.
Organizer cells have been studied for decades, with University of Freiburg Ph.D. candidate Hilde Mangold conducting the first experiment in 1921 under advisor Hans Spemann. Their detection of the “Spemann-Mangold organizer”—a group of cells found in an amphibious embryo that initiates the central nervous system’s formation—facilitated the study of tissue induction by embryologists. This analysis of how cells shape the development of other cells and tissues led many to examine the organizers found in different species, but national scientific guidelines prevented scientists from studying the human embryo past 14 days (a timepoint chosen due to the emergence of the primitive streak, a strip of tissue that forms prior to human embryonic brain development.) This “14-day rule” was adopted by the National Institutes of Health’s Human Embryo Research Panel in 1994 and is currently being challenged by scientists wishing to conduct further studies on more developed embryos.
Rockefeller University’s lead researcher Ali Brivanlou and his team identified the self-organizing potential of human embryos in May 2016 but ended their experiment before embryonic cells began the process of primitive streak development, thus being unable to detect the human organizer prior to their 2018 study.
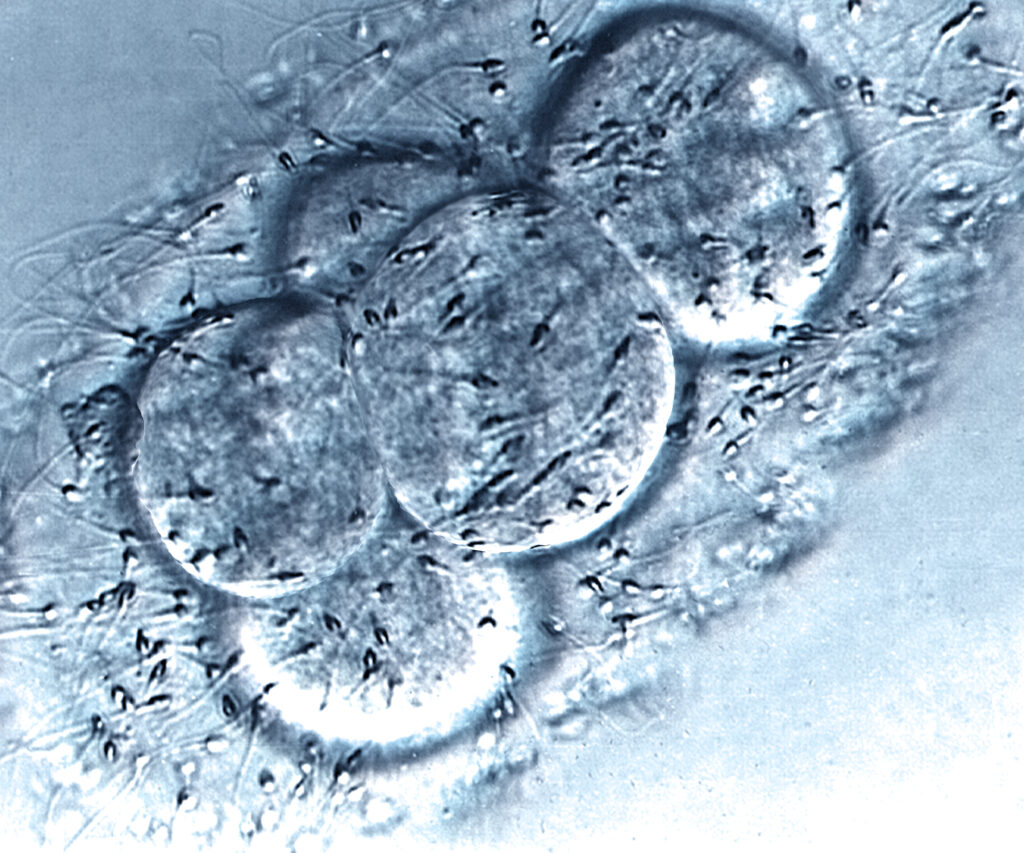
According to Brivanlou, the scientists skirted the 14-day rule by forming gastruloids—human embryo-like structures—from embryonic stem cells. The scientists cultured these cells on 22-millimeter squares to control their growth and shape. After they were given the protein BMP4, the gastruloids then began to create the germ layers indicative of early embryonic development. When the proteins WNT3A and Activin were used as stimulants to trigger the development of an organizer and primitive streak—two characteristics of early gastrulation—Brivanlou and his team later grafted them into 12-hour-old chicken embryos. Similar to two-week-old human embryos, these allowed the scientists to observe their interactions with the human organizer cells.
The result? Guided by the organizer formed by the human cells, the chicken cells created a secondary developmental axis in each embryo, which later formed a second nervous system. This development confirmed the existence of the human organizer and its defining trait. Moreover, the secondary axes’ “self-organizing features” and non-autonomous creation of neural tissues by the human cells upheld that WNT3A and Activin aid in the organizer’s creation.
Scientists are hopeful that the study on these hybrid embryos and identification of the human organizers can be used to develop cures for conditions like Huntington’s disease, better understand fetal development, and aid in miscarriage prevention through further examination of human embryology. They anticipate that future experiments centered on how other cells are directed by these human organizers may lead to new breakthroughs in using human stem cells to produce tissues for regenerative medicine. Researchers also argue that the experiment paves the way for more ethical procedures in stem cell research because the study did not utilize human embryos.
The participating scientists assert these hybrid embryos will be used exclusively to study diseases instigated by mutant genes that can be identified during embryonic development. Yet Brivanlou opposes the notion that his experiment negates a need for further research to be done on human embryos themselves.
“There is no substitute for studying the real embryo,” he insists. “Everything else we do when we try to model kind of oversimplifies it.”
The scientist isn’t satisfied with an alternative—and he isn’t the only one.
Some researchers argue the 14-day rule is a restriction that ultimately hinders them from finding cures and developing new stem cell therapies. In 2017 bioethicist Insoo Hyun argued that given their proposed eventual destruction, utilizing embryos “left over” from procedures such as IVF treatments should be permitted. He also addressed the ambiguity of certain embryological studies, saying:
“At what point is your model of an embryo basically an embryo? Are we creating life that, in the right circumstances, if you were to transfer this to the womb it would continue its journey?”
His concerns are hardly surprising to other scientists. The original lack of consensus on human embryos’ moral status ultimately led to the current guidelines for scientific research. The 14-day rule was established not to assert what protections and rights should be afforded to them, but rather to limit research before more “morally troubling” traits—sentience, the ability to survive and grow outside the womb, and fetal heartbeat detection—developed. Though it has been lauded by some scientists as an effective stopping point, the guideline does not definitively address the biological reality of human embryos—or acknowledge recent developments such as human chimeras. Moreover, if development of embryo-like structures progresses in future research, their “self-organizing features” may result in their reclassification as “synthetic” embryos with the potential for further growth. As ethical standards become increasingly uncertain, some scientists question whether these embryoids should be excluded from the existing research guidelines.
Ethical Implications of Hybrid Embryos
Rockefeller University’s use of human embryonic stem cells to study the gastrulation process, and its transplantation of one species’ cells into the embryos of another, ultimately undermined ethical standards in research because it required the destruction of early human life when the scientists derived the embryonic stem cells from human embryos in the first place.
The result—interspecies embryos—raises other ethical dilemmas that health policy has yet to address. Brivanlou’s team state their human-chicken chimeras were not permitted to hatch and will be used solely for research purposes. Moreover, they asserted the transplanted human cells constituted just 10 percent of each hybrid embryo during its development. But human nature inevitably encourages further inquiry. Other scientists have proposed the transplantation of hybrid embryos into female livestock’s wombs for further development and eventual harvesting of organs and tissues. Such procedures fail to provide adequate protections for embryos with an unmistakably human component.
Brivanlou’s findings invite yet another concern—scientists often maintain that a human embryo’s moral status is not absolute but rather a condition that is acquired as development progresses. Such a belief does not adopt a concrete stance on human life and must be readdressed as the humanity of embryoids and human chimeras poses new questions for scientific research.
Sara Allocco is an intern for the Charlotte Lozier Institute.