Charlie Gard’s Case and Parental Advocacy for Chronically Ill Children
“My biggest issue is this: a parent is a caregiver and then of course the health professionals are the caregivers, but you know, who gets the final say?”
-Mother whose daughter has osteosarcoma
This essential question was posed by the mother of one of 33 children living with chronic conditions whose parents I interviewed for my recently published study in the current issue of Health Communication. The study is titled, “You know the medicine, I know my kid”: How parents advocate for their children living with complex chronic conditions.
Twelve of the 33 children were living with rare genetic conditions that had an unknown prognosis or required life-long care. Interviewing 35 parents, I found that parents’ advocacy roles are a complex communicative process that extends beyond simple chronic disease management and transcends across multiple settings simultaneously (hospitals, schools, social media, family). To put it simply, advocacy is another type of work that parents of chronically ill children must assume alongside daily life responsibilities (e.g., working, tending to other children), as well as new and unexpected responsibilities, such as tube feeding or coordinating appointments. Altogether these responsibilities result in parents, on average, spending an extra 30 hours per week tending to the needs of their child’s chronic illness (National Alliance for Caregiving & American Association for Retired People [AARP], 2009).
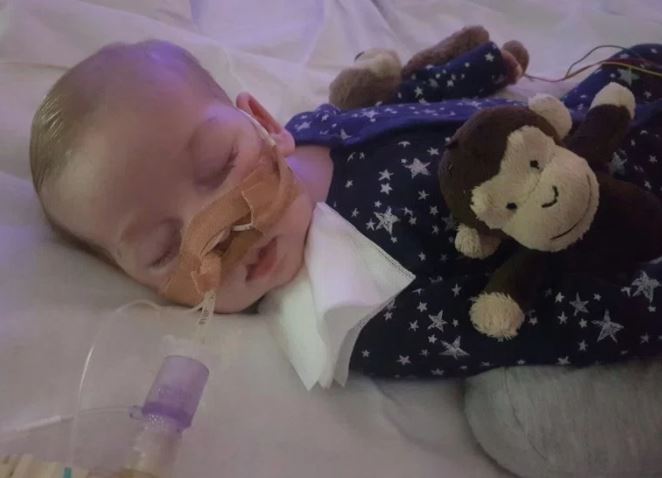
My study is especially timely given the recent media attention to the Charlie Gard case. Eleven-month-old Charlie was born with encephalomyopathic mitochondrial DNA depletion syndrome, a rare and typically fatal genetic condition. His parents, Connie Yates and Chris Gard, have been in a long legal battle with London’s Great Ormond Street Hospital over their differences regarding the best treatment for Charlie. The hospital believes that the best decision is to remove life support, which would ultimately end his life. Charlie’s parents oppose this decision and have personally raised ~$1.7 million in private funds to help finance experimental treatment in the United States, which they believe could save his life. Despite the parents’ wishes, three British courts and the European Court of Human Rights have sided with the hospital. The most recent ruling from the European Court said: “It was most likely Charlie was being exposed to continued pain, suffering and distress, and that undergoing experimental treatment with no prospects of success would offer no benefit, and continue to cause him significant harm.”
Coming down on the opposite side, Charlie’s case has been championed by such figures as the Pope and the President of the United States, who have both expressed solidarity with his parents and the hope that something more can be done to help the little boy.
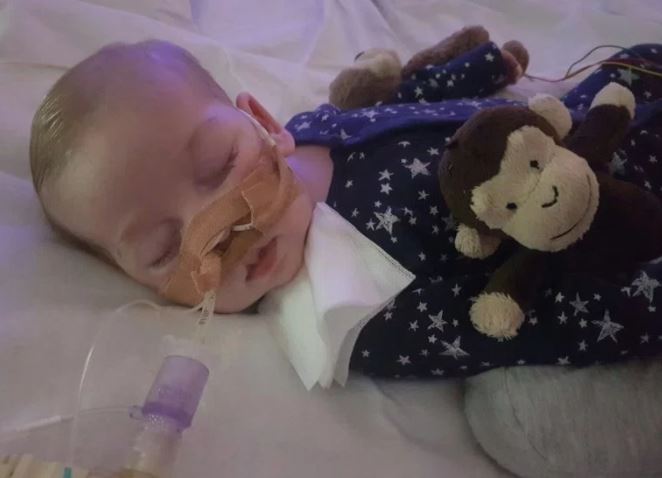 photo credit : bit.ly/2tPWn6m
photo credit : bit.ly/2tPWn6m
If the international attention surrounding Charlie’s case is somewhat unusual, the challenges his parents have faced are common and resonate across national boundaries. Today, one in 5 North American children are diagnosed with a chronic condition (Boyse, Boujaoude, & Laundy, 2012). That means as many as 30 million parents may be tasked with the responsibility of being their sick child’s primary advocate. My study shows the complex balancing act that takes place as parents become experts in advocating for their chronically ill child. In particular parents described advocacy as a task that included behaviors such as: establishing roles and responsibilities across team members (e.g., extended family, friends, healthcare professionals), fostering relationships within one’s social network, and staying informed, so as to effectively coordinate their child’s care team and advocate on his or her behalf.
One of the most demanding aspects of parental advocacy, as we see in cases like Charlie Gard’s and in my study, is the emotional labor. In my interviews, parents described the challenges of negotiating roles with medical providers, as well as experiencing social stigma and receiving limited access to knowledge and expertise. Some parents reported being in an adversarial relationship with health professionals as they encountered conflict or received little support, as one mother whose daughter had cancer stated: “You have got these health professionals who want what is best for the child and what if that conflicts with what a parent thinks is best for the child? Who does the parent go to then? Because I am hearing stories about people who are getting their kids taken away because they do not comply with the hospital’s rules.”
The reality of the fears and frustrations expressed by this mother is illuminated to the whole world through cases like Charlie Gard’s. If parents’ primacy as caregivers and their wishes for their child’s treatment are not respected, ultimately it is not only the relationship between parents and health professionals that breaks down, but the quality of care the child receives is likely to suffer as well.
Dr. Katherine Rafferty, Ph.D., M.A. is an Associate Scholar of the Charlotte Lozier Institute since Fall 2016. She is a lecturer at Iowa State University, and previously worked as a Health Communication Specialist for the Centers for Disease Control and Prevention (CDC). She conducts research that lies at the intersection of interpersonal and health communications with a focus on how patients and families manage and cope with chronic illness and end-of-life care. For a recent Q&A with Dr. Rafferty on her expertise, please see: https://lozierinstitute.org/qa-with-the-scholars-discussing-chronic-illness-and-end-of-life-care/