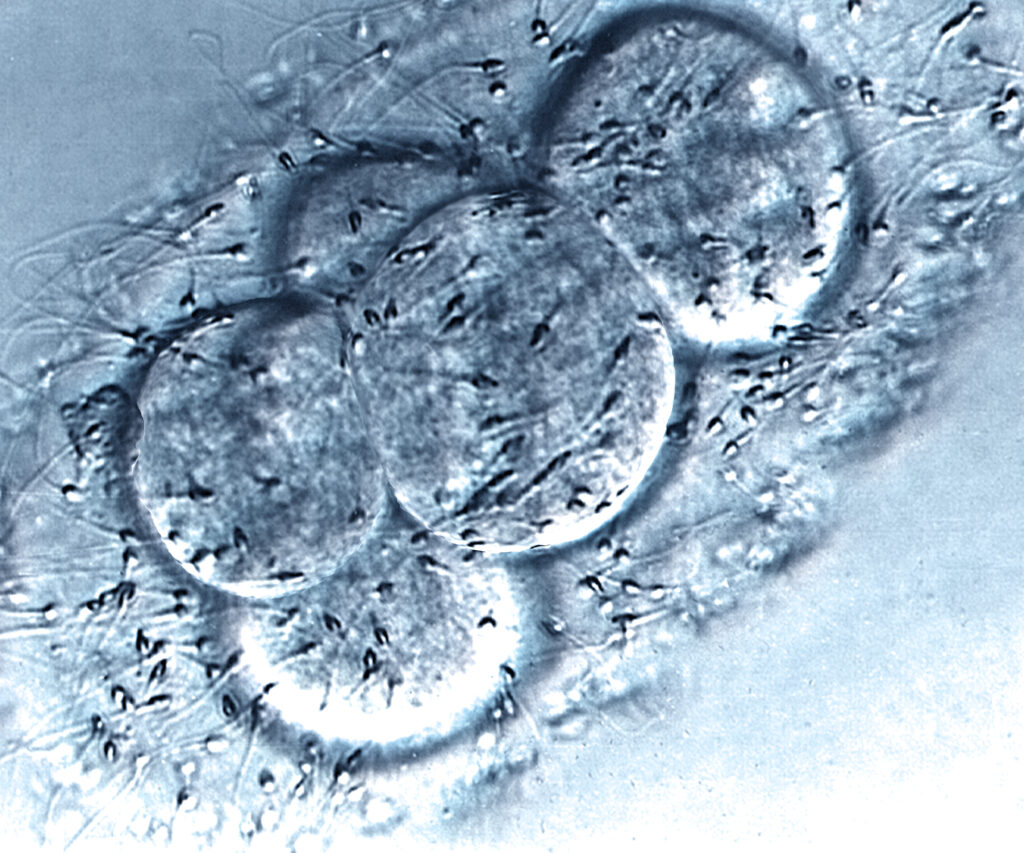
iPSCs: A New Gold Standard in Regenerative Medicine?
A recent press release from the National Institutes of Health calls attention to a study, published in Stem Cell Reports, that researchers have “developed a clinical-grade stem cell line, which has the potential to accelerate the advance of new medical applications and cell-based therapies for millions of people suffering from such ailments as Alzheimer’s disease, Parkinson’s disease, spinal cord injury, diabetes, and muscular dystrophy.” The development of these clinical grade stem cells, the release notes, “removes a significant barrier in the development of cell-based therapies.” But is NIH’s promotion of “stem cells” anything new?
Since human embryonic stem cells (hESCs) were first isolated and successfully grown in culture in 1998, they have been hyped as opening up a new age for medicine, and having a virtually unlimited potential to cure any number of diseases and conditions, including all of those listed above and many more.
The late Senator Arlen Specter said (at page S2764) hESCs “could result in a veritable fountain of youth by replacing diseased or damaged cells.” When President Obama expanded federal funding for stem cell research, then-House Speaker Nancy Pelosi waxed theological, musing that “Scientists have been given an almost biblical power to cure through advances in embryonic stem cell research.”
Patient advocacy groups such as the Alliance for Aging said that hESC research allows us to “imagine a world without debilitating costly diseases such as Parkinson’s, heart disease and diabetes.” Celebrities, most notably Michael J. Fox and the late Christopher Reeve, appeared before Congress to hype the potential of hESC research. Fox stated outright that hESC research has the “potential to eliminate diseases, literally save millions of lives,” while Christopher Reeve told a Senate committee, “For the true biological miracles that researchers have only begun to foresee, medical science must turn to undifferentiated [embryonic] stem cells.”[1]
So there is really nothing new that the NIH should be promoting the therapeutic potential of stem cells so lavishly in its news release.
But what is new here is that the stem cells that the NIH release hails as having “the potential to accelerate the advance of new medical applications and cell-based therapies for millions of people,” and thus “removes a significant barrier in the development of cell-based therapies,” are not embryonic stem cells. They are non-embryonic, induced pluripotent stem cells derived from human umbilical cord blood cells.
The NIH explains that “these clinical-grade stem cells are different from the more common laboratory-grade cells those (sic) used in most scientific publications because unlike laboratory-grade stem cells, clinical-grade stem cells can be used for clinical applications in humans. The distinctive feature of this cell line is that it was developed under current good manufacturing practices (cGMP), a set of stringent regulations enforced by the U.S. Food and Drug Administration which ensures each batch of cells produced will meet quality and safety standards required for potential clinical use.”
This development—and especially NIH’s take on it—amounts to a virtual sea-change in the alleged scientific “consensus” that hESCs are the gold standard for research in regenerative medicine. Reading the NIH release, it’s fair to conclude that ethically non-contentious, non-embryonic stem cells are now leading the way and showing greater potential in developing clinical trials and, hopefully, cures.
Of course, caution should be exercised regarding these developments. Non-embryonic stem cells must not now become subject to the same type of hype and exaggerations that once surrounded hESCs and that led to such disappointment among patients.
Ethically non-contentious, non-embryonic stem cell research offers real hope.
It does not need the hype.
Gene Tarne is Senior Analyst for the Charlotte Lozier Institute.
[1] Testimony before the Senate Committee on Appropriations, Subcommittee on Labor, Health and Human Services and Education, 4/26/00