Q&A with the Scholars: The Science of Fetal Pain
Sheila Page, D.O., is board certified in Neuromusculoskeletal Medicine and Osteopathic Manipulative Therapy. She treats a wide spectrum of patients from the newborn to the elderly, including patients with irreversible and terminal illness. Dr. Page has a special interest in children with disabilities, particularly those whose burden of care is difficult and who have been given little hope for a better quality of life. Dr. Page is one of our nearly 40 associate scholars. In this interview, she discusses palliative care and the science of fetal pain.

In your practice of medicine, you have worked with patients of various ages who are experiencing pain and who in some cases have serious, irreversible medical conditions. How do you seek to improve quality of life for these patients, and does your approach to treating your young patients differ from those who are older?
Page: Over the past 23 years, I have seen a broad spectrum of patients, including those who have either acute pain or breakthrough pain in chronic or terminal conditions. My goal is to help the patient to become pain-free or to improve their quality of life. Using osteopathic manipulative treatment, I try to increase mobility, decrease pain, and improve functions such as breathing, especially when the patient suffers from lung congestion or chest wall pain with breathing.
Using osteopathic manipulative medicine, I balance tensions in the fascial and tendinous elements of the body, relieving strains and congestion. The way I treat healthier adults is different than my approach to very frail patients, or children and infants. Sometimes, in order to resolve the problem, I have to directly touch painful areas, initially causing some pain. That discomfort usually resolves with successful treatment and the patient immediately feels relief. With children, I have to be very gentle and patient. They often are already in pain and at first are pretty upset about my treatment. Once they feel relief, however, they understand and are usually eager to be treated.
What definitions of pain are operative in your profession, and how do those definitions come into play in your experience treating patients who are trying to come to grips with suffering?
Page: My patients often come to me hoping to minimize or eliminate the need for drugs. When someone tells me he or she is suffering, I take it seriously, regardless of whether I am immediately able to identify a cause or solve the problem. I find that it puts the patient at ease when they realize they don’t have to prove anything to me before I will treat them. I recognize that pain and suffering cause them to seek help from me. The many complicating variables that contribute to the pain a person experiences are all considered as I work with them, first addressing the physical pain that they experience and its root cause.
When does the unborn child begin to respond to sensory input and become capable of feeling pain? How does the formation and functioning of the nervous system factor into this capacity?
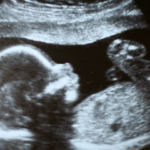
Page: The unborn child responds to sensory input as early as seven weeks (gestational age). All of the organ systems of the developing human demonstrate function simultaneously with the appearance of the anatomical structure. By 10 weeks, the human embryo has well-developed organ systems and most of the anatomy can be named with the same nomenclature that we use in adults.[1] The brain has been growing rapidly and will continue to develop as the baby grows, moves, and experiences the sensory input of the environment surrounding it. There is no point in development in which the structure exists without function.
With respect to the nervous system, the structures responsible for pain perception are the afferent and efferent nerves and the lower brain structures, including the reticular activating system and the thalamus. There is no pain perception center in the cortex—the pain fibers all terminate in the reticular activating system, and a very small percent will connect in the thalamus to neurons that travel to the cortex for the purpose of localizing the pain. At seven weeks, the thalamus is visible. Within a few days, the entire system of pain perception expands into a completely intact structure and continues to develop into a very sophisticated part of the nervous system.
What are the most common arguments against providing pain prevention for the unborn child? What do you think is the motivating force behind these arguments?
Page: I can’t begin to understand a motivating force behind insisting that pre-born children feel no pain. The arguments are often centered on a false supposition that there is a pain perception center in the cortex that is not functioning or intact until as late as 26 weeks. There is simply no evidence that this is true. Almost all of the pain fibers terminate in the reticular activating system, and a small percent connect in the thalamus to neurons that travel to the sensory motor cortex for the purpose of localizing the pain. This means that the message is delivered to its intended destination, the lower brain centers, which are responsible for the perception of pain and for alerting the whole nervous response system that damage has been inflicted.
Other arguments dismiss the fact that surgeons who care for babies in-utero during fetal surgery and other interventions use anesthesia and analgesic drugs on their tiny patients. They casually state that, in the context of abortion, the use of anesthesia would be solely for the “beneficence” of the pre-born child, and therefore would not apply. Since abortion is not a procedure that is intended to benefit the child in the first place, they have no reason to try to discern whether the victim suffers in the process.
Why are you pro-life? If you had 60 seconds to explain to someone why you have pursued the work that you have throughout your career, what do you tell them?
Page: I love the practice of medicine, and especially love the relationship of trust that I have been able to develop with my patients. I am drawn to children with disabilities and patients who have debilitating disease that is chronic or end-stage. The opportunity to give them comfort and to improve the quality of their lives is a privilege to me. The focus of my specialty on the neuromusculoskeletal system made it natural for me to take on the research of the development of pain perception in the human embryo.
I have become convinced that innocent human life must be protected. Denying the humanity of the pre-born child is a terrible deception, and justifying its destruction, as if the pre-born are less than human and the property of another, diminishes and confuses our understanding of our own origin. I have heard the testimonies of hundreds of women, on both sides of the abortion debate. It is clear to me that everyone instinctively recognizes that human life is present at the moment of conception. If not, there would not be such a desperate and highly organized effort to destroy it and justify the right to do so.
Dr. Page’s full biography can be found here.
[1] See Derbyshire SW, Foetal Pain?, Best Practice & Research Clinical Obstetrics and Gynaecology (2010), doi:10.1016/j.bpobgyn.2010.02.013. See also Lowery, C. MD, Neurodevelopmental Changes of Fetal Pain, Seminars in Perinatology 31(2007) 275-282. See also Salihagic Kadic, A, Predojevic, M., Fetal Neurophysiology according to gestational age, Seminars in Fetal and Neonatal Medicine (2012), doi. 10.1016/j.siny.2012.05.007.