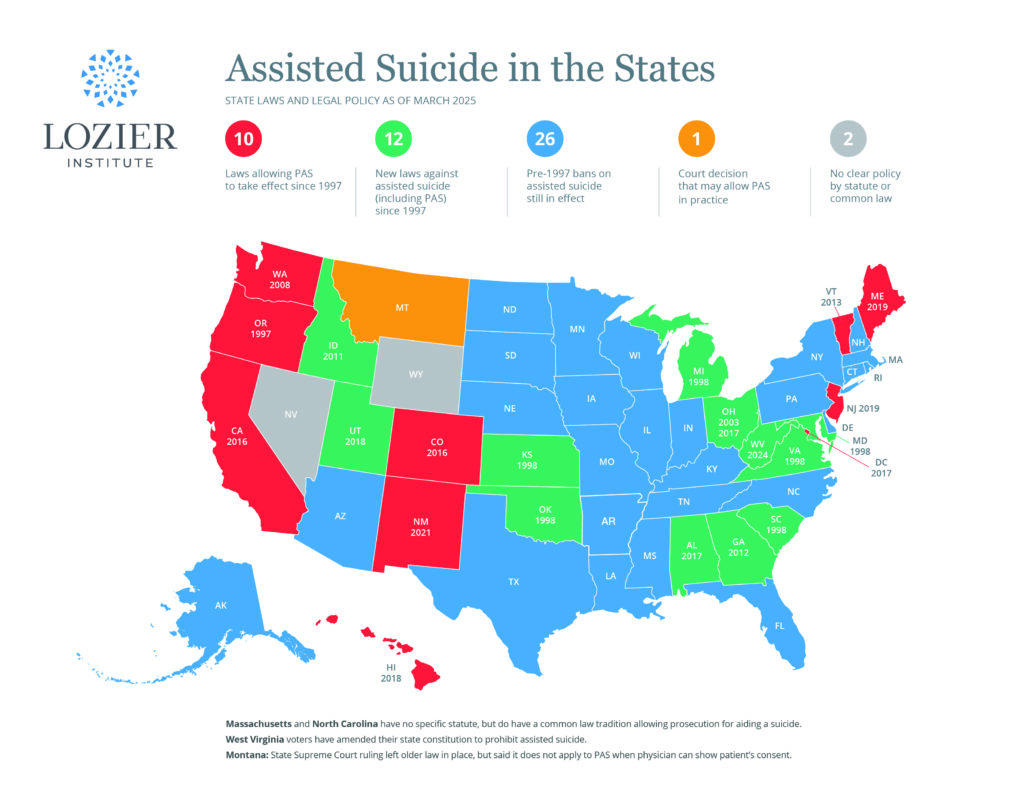
States Consider Assisted Suicide in 2016 as New JAMA Study Raises Concerns

Already this year, at least eight states are considering bills to legalize physician-assisted suicide. Of these, Colorado, Maryland, and Utah have renamed their bills, formerly titled “Death with Dignity,” as “End of Life Options” bills – the name under which California legalized assisted suicide last October.
Yet, the deceptive title, which now eliminates all reference to death, seemingly seeks both to legalize and normalize assisted suicide as “just another medical option.” A new study published last week in JAMA Psychiatry, however, raises afresh ongoing concerns with assisted suicide, especially as it relates to those with mental illness or distress.
The study, led by National Institutes of Health psychiatrist and bioethicist Dr. Scott Y.H. Kim, covered 2011 to 2014 and examined all published cases in the Netherlands of euthanasia or assisted suicide for psychiatric conditions. (The Netherlands, Belgium, and Switzerland allow assisted suicide for mental suffering.)
The findings from these 66 cases paint a tragic picture of the patients who died from euthanasia or assisted suicide:
- 80 percent had previously been hospitalized for psychiatric reasons
- 52 percent had previously attempted suicide (non-assisted)
- 58 percent had at least one other medical condition
- 55 percent had depressive disorders as the primary psychiatric issue
- 56 percent of the physician reports mentioned the patients’ social isolation or loneliness
- 56 percent had refused some treatment
An overwhelming 70 percent were women. One cannot highlight enough that most of these individuals were vulnerable to suicide due to depression and feeling alone. That more than half of these patients had tried to commit suicide on their own previously, and then succeeded by way of a legal process involving healthcare providers, is alarming.

Striking descriptions of the vulnerable mental state of these patients, as reported by the physicians, include a woman who “indicated she had had a life without love and therefore had no right to exist” and a patient who was an “utterly lonely man whose life had been a failure.”
Depression also seemingly played a part in many of these individuals refusing treatment of some sort. The study significantly notes that while most did have extensive treatment histories over time, most also had refused some kind of treatment – half of those refusing due to “no motivation.”
On the other end of the spectrum was one woman in her 70s who, according to the study, was “without health problems” and whose consultant reported that she “did not feel depressed at all. She ate, drank, and slept well. She followed the news and undertook activities.” The reason for her seeking death – and for which she was given it apparently – was that her husband died a year prior and they promised each other that one would not live without the other, said the study.
Another troubling aspect of the study showed that for more than a quarter (27%) of cases, the doctor performing euthanasia or assisted suicide was new to the patient, and in most of these cases, affiliated with a particular mobile euthanasia clinic funded by a euthanasia advocacy organization.
In a New York Times article published last week on this study, Dr. Paul Appelbaum, professor of psychiatry, medicine, and law at Columbia University, stressed the problem of this arrangement, saying, “The idea that people are leaving their treating physician and going to a clinic that exists solely for this purpose, and being evaluated not by a psychiatrist but by someone else who has to make these very difficult decisions about levels of suffering and disease – it seems to me like the worst possible way of implementing this process.”
“Doctor-shopping,” as it is commonly called, has long been a concern for those against assisted suicide and euthanasia, and rightly so, as it has its own record of abuses in Oregon, the first American state to legalize assisted suicide in 1997.
As for any supposed “better way to implement the process” (assisted suicide and euthanasia), a record of the slippery slope in countries in Europe and lists of recorded abuses in Oregon and Washington state show that any purported safeguards can be circumvented, ultimately making restrictions unenforceable.
Even judging a person’s legal “eligibility” for assisted suicide or euthanasia proves tricky as evidenced by the disagreement among patients’ physicians for 24 percent of the cases in the JAMA study. That is, the patients had multiple physicians involved in their cases, and their doctors disagreed among themselves about whether the patients met the criterion for “unbearable suffering,” “competence” and “futility” in a full quarter of cases. Yet, disturbingly, the study says, “EAS [euthanasia or assisted suicide] proceeded with the disagreements unresolved for most cases.” (Emphasis added.)
Despite this study’s significance, some advocates of euthanasia and assisted suicide in the United States will continue to claim that the Netherlands’ situation, or even the debate on assisted suicide for mental illness itself, has no bearing in the United States because our bills, modeled after Oregon’s, do not permit it on grounds of mental distress.
However, Oregon’s law and the at least eight bills pending for 2016 do not require that any kind of mental health screening be given as a basic prerequisite after a person requests assisted suicide. Instead, Oregon’s law states that the physician “shall refer the patient for counseling” only “[i]f in the opinion of the attending physician or consulting physicians a patient may be suffering from a psychiatric or psychological disorder or depression causing impaired judgment” (emphasis added).
But would it not be challenging for doctors to suspect mental health problems if the patient were new to them and there were no baseline reference established for the person’s affect? In fact, official state data published recently for Oregon’s assisted suicide law in 2015 shows that the median period of a doctor-patient relationship was only nine weeks (10 weeks less than last year).
More to the point is that the new Oregon report shows only five percent of all people (52 of 991) dying from assisted suicide since the law went into effect 18 years ago were referred by the doctor for psychiatric evaluation.
Taken in the context of Oregon’s disturbing track record of failure to refer patients who died of assisted suicide for mental health evaluation or counseling, the Netherlands JAMA study does bear a warning to the states currently considering it. As the American Medical Association states, assisted suicide “is fundamentally incompatible with the physician’s role as healer” and “patients should not be abandoned.” The time is ripe for disability rights groups, advocates for the elderly, medical groups, faith communities, and pro-life groups among others to continue working together to educate on the harms of assisted suicide, oppose the practice, and seek true medical care for the vulnerable and suffering among us.
Genevieve Plaster is a research assistant for the Charlotte Lozier Institute.