Fetal Surgery: Hope for Families and the Patient in Utero
January is National Birth Defects Prevention Month. In the United States, about 120,000 babies each year have a congenital anomaly, otherwise known as a birth defect, according to the Centers for Disease Control. That is, about one in every 33 babies is diagnosed either prenatally or after birth with a health problem or physical abnormality that varies in degree of severity. Severe birth defects account for one out of every five infant deaths, making it the leading cause of infant mortality.
For parents who receive the heartrending news that their unborn child has a severe or life-threatening fetal anomaly, fetal surgery – surgery performed on a child in the womb – is one option that offers hope.

The Srinivasans can testify to that. In 2007, Michigan couple Laura and Reuben Srinivasan learned at a routine 19 weeks ultrasound that their unborn daughter had a solid chest mass developing between her heart and lungs. Their physician stated that her case of mediastinal teratoma was “a fatal thing” and presented them with the options of aborting their daughter or waiting for her to die in utero and then delivering her. “We were totally distraught,” said Mrs. Srinivasan. “She hadn’t been born yet; we didn’t even know her, yet we had all these high hopes for her. Everyone was saying it was fatal. We had to do everything we could, we had to exhaust all possibilities.”
Resolved, the Srinivasans opted for a third alternative: fetal surgery. At just 23 weeks gestation – just over halfway through pregnancy – fetal surgeons at the Children’s Hospital of Philadelphia (CHOP) operated on their daughter in the womb to remove the growth. While the surgery to remove the tumor was successful, Grace was born very prematurely only a few days later. Mrs. Srinivasan described the desperate situation, saying, “The doctors in the N/IICU said she was one of the sickest babies they had ever seen.” Yet with their loving care, baby Grace survived, and as of 2009 she was a healthy, normally developing two-and-a-half-year-old.
The Srinivasan’s story is just one among an ever increasing anthology of hope. This year in fact, CHOP celebrates the 20th anniversary of its Fetal Surgery Program, which has performed a record-breaking 1,200 prenatal surgeries.
In a recent interview, Dr. Scott Adzick, CHOP’s Surgeon-in-Chief, explained the significance of fetal surgery by way of a much-cited study he co-led known as the MOMS Trial (Management of Myelomeningocele Study). The study compared the health outcomes of children with spina bifida who underwent surgery in utero and those who underwent surgery after birth. “[D]irect comparison showed that the fetal surgery group did better in almost every way [than the postnatal care group]. Specifically, the fetal surgery group had improved nerve and leg function, improved ability to walk, and decreased need for a shunt tube to drain hydrocephalus…. It definitively showed the benefits of the fetal surgery in the most rigorous test.”
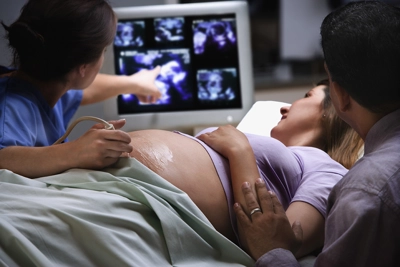
Though fetal surgery is not yet as widely available as it is needed due to its complexity, it has been performed for decades. The first recorded successful human fetal intervention was an intrauterine blood transfusion performed in 1963 in New Zealand; however, it was two more decades before safer anesthetic and surgical techniques were developed. By 1981, Dr. Michael Harrison at the University of California-San Francisco performed the first successful open fetal surgery on an unborn child with spina bifida, paving the way for the subfield of fetal surgery. Since then, new technologies have continued to develop that allow for less invasive interventions such as fetal image-guided surgery. FIGS-IT, as it is also known, may be done with only a local anesthetic for the mother, and uses a sonogram in real time to guide a needle to the child in utero for repairing milder conditions.
By way of returning to the prevention of birth defects, let us consider the rather straightforward question and answer below:
Did you know that an unborn child is not always protected from the outside world?
Fact: The placenta, which attaches a baby to the mother, is not a strong barrier. When a mother uses cigarettes, alcohol, or other drugs, or is exposed to infectious diseases, her baby is exposed also. Healthy habits like taking folic acid daily and eating nutritious foods can help ensure that a child is born healthy.
This fact sheet that refers to an “unborn child” and a “baby” waiting to be born was published by the Department of Health and Human Services and the Centers for Disease Control (whose motto, incidentally, is “Saving Lives, Protecting People.”)
Whether it intends to or not, National Birth Defects Prevention Month will always bring to the fore the delicate beginnings of the developing baby and her relationship with her mother. With each life saved, the field of fetal surgery progressively phases out the relevance of the “abortion-or-miscarriage” conversation that often follows a diagnosis of a potentially life-threatening fetal anomaly. As the March for Life nears, may the “prevention” and intervention of fetal anomalies be pursued only with regard to the anomalies, and never with respect to the lives of these tiniest of patients!
Genevieve Plaster is a Research Assistant for the Charlotte Lozier Institute.