Massachusetts’ “Death with Dignity” Initiative: Questions Regarding Question 2
By Jacqueline H. Abernathy, Ph.D.
Download PDF here: Massachusetts’ Death with Dignity Initiative_Questions Regarding Question 2
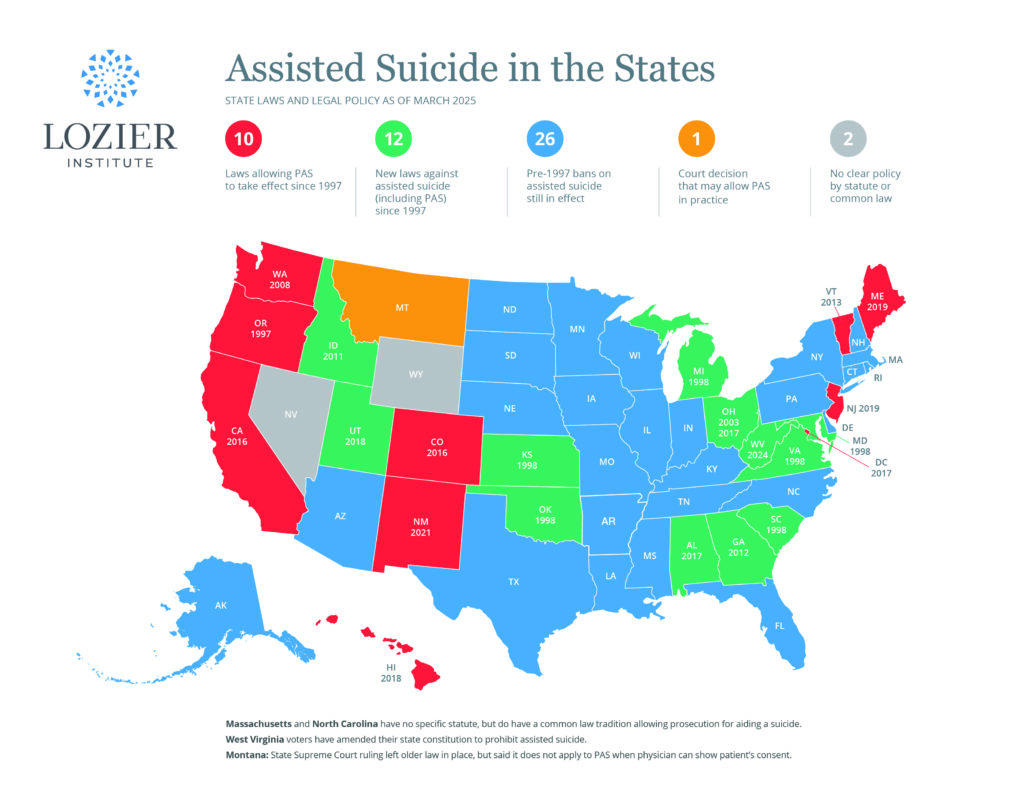
The 2012 “Act Relative to Death with Dignity” goes before Massachusetts voters on November 6. Question 2 asks voters directly whether to legalize physician-assisted suicide (PAS) or uphold existing state statutes. If voters affirm Question 2, Massachusetts would join Oregon, Washington and Montana as the only states in the U.S. to allow this practice. Recent studies on PAS in these states paint a revealing portrait of what would transpire in Massachusetts if voters approve Question 2. However, unlike citizens of Oregon who passed the first “Death with Dignity Act” in 1997, voters in Massachusetts have the benefit of learning the actual outcomes of such legislation in other states. Voters now have access to numerous studies that both vindicate opponents’ predictions about PAS and present even more concerns.
Concern 1: Denial of Palliative Care Coverage
Oregon and Washington impose reporting requirements for PAS, and while there are only three years of data from Washington (Washington’s “Death with Dignity” Act took effect in 2009), objective studies done in both states support many of the fears listed by opponents of Massachusetts’ “Death with Dignity” Initiative. Opponents predicted in 1997 that states that legalize PAS may coax and coerce unwilling patients toward ending their lives by limiting or denying palliative care. While PAS proponents have since cited increased spending on palliative care as evidence that opponents were incorrect, other reports confirm opponents’ fears, particularly incidents where terminally ill citizens were told by state medical plan authorities that they would not pay the cost of pain-control, but would cover the cost of their suicides. Another study indicated that 24 percent of patients who chose PAS reported that they did not have adequate finances to cover expenditures for medical care and equipment, in spite of the fact that 98 percent of respondents had health insurance. Fears that PAS may not be freely chosen by patients but instead represent a last act of desperation are supported by this evidence.
Concern 2: Inheritance and Other Financial Incentives
PAS proponents attempt to refute opponents’ claim that PAS would disproportionately target the vulnerable, citing the fact that people who have taken their own lives are better educated and more financially stable than the general population. Opponents reply that this highlights another grave concern, financial abuse of the elderly, suggesting that those patients who have a significant estate may feel compelled to die in order to leave their property to their heirs. A recent study of patients receiving PAS in Oregon and Washington demonstrates that PAS may not be used to benefit the patient, but the patient’s family. One study employed a “Quality of Death and Dying Questionnaire” that examined patient pain and other symptoms as well as readiness for death, anxiety and mood[1]. The study indicated that patients choosing PAS did not report a higher quality of death than those dying naturally, but rather that the patient’s family members did indicate a higher quality of death on some items. Additional research also found that caregivers of patients in both Oregon and Washington who ended their lives by PAS were themselves suffering from substantial financial and health-related harms: 37 percent had lost income because of caregiving (18 percent had had to quit their paying jobs), 12 percent had become ill themselves while caregiving, 29 percent had delayed plans for themselves or their families, 23 percent stated that their social lives suffered frequently, 20 percent complained that they often did not have enough time for themselves, 33 percent frequently felt stressed because of caregiving, and 24 percent were clinically depressed. Although respondents claim that none of these factors was associated with the decision to end the patient’s life, Washington State reported in 2011 that over half of respondents choosing PAS mentioned “concerns about being a burden” as a reason for choosing to take their own lives. This evidence overwhelmingly suggests that opponents’ fears of patient coercion are well-founded and that patients may not choose PAS in their best interest, but rather in the perceived best interest of others – many of whom stand to gain from a patient’s earlier demise.
Concern 3: Adverse Impact on the Disabled
Additionally, an exhaustive analysis of 11 years of reports on Oregon’s statute failed to quiet the ongoing outcry regarding the possibility that PAS unduly targets persons with disabilities. This panel of scholars examined all available literature on Oregon’s Death with Dignity Act and ultimately determined that physicians may bias their assessments of the quality or worthiness of life with a disability and influence the recommendation regarding life-sustaining treatment options. The authors agree with many opponents of PAS who note the potential for abuse due to the lack of oversight of or penalties for rogue physicians who choose not to report assisted suicides to the proper authorities.
Concern 4: Mistaken Diagnoses and Life Expectancy
Along with a lack of oversight and accountability for physicians, a review of studies also determined that physicians’ medical diagnoses were often incorrect, both in declaring a patient to have a terminal condition and estimating their life expectancy at six months or fewer. A prognosis of only six months equals 180 days maximum, and yet Oregon’s report indicates the number of days between writing the lethal prescription and the patient’s actual death ranged from zero to 698 days (nearly two years). Another study of physicians who were willing to prescribe the lethal dose found that 27 percent were not confident that they could determine if a patient only had six months or fewer to live. One report discusses a PAS opponent from Oregon who was told that she had only six months to one year to live; today, over 11 years later, she is still alive. Additionally, since many people survive in spite of terminal prognosis, and since the median number of days between the writing of a lethal prescription and the patient’s death is seven, it is unknown how many of these patients would have actually died within the six-month timeframe or anything close to it. There is also the report that many patients opting to end their lives suffer from treatable depression and physicians report that patients for whom interventions were made (like treating depression) were more likely to change their minds about wanting to end their lives. One analyst, after examining Oregon’s most recent annual report, found that physicians who prescribe the lethal medications are failing to refer for necessary psychiatric evaluations of patients, many of whom might reconsider suicide if properly treated. This prompts the question of how many people freely choose PAS or are pressured into the decision by negative circumstances, especially circumstances for which there is some or complete relief.
Concern 5: Medico-Professional Opposition to PAS
Despite media portrayals of opposition to PAS as based primarily on moral or religious grounds, data reaffirms that the most enduring opponents of PAS are physicians. The American Medical Association has not wavered in its opposition to PAS and states, “Physician-assisted suicide is fundamentally incompatible with the physician’s role as healer, would be difficult or impossible to control, and would pose serious societal risks.” The medical community’s staunch opposition to PAS is regarded as a major reason why no state legislature has legalized PAS despite more than 120 attempts, as overwhelming expert testimony against this practice has succeeded in persuading legislators across party lines of its demonstrated dangers. Legislative attempts failed in Montana in 2009, where PAS was only legalized by court decree. Indeed, ballot initiatives were approved in Oregon (1994) and Washington (2008), following years of failed legislative attempts. Likewise, proposed bills failed in the Massachusetts legislature in 1995, 1997, 2009 and, most recently, 2011 and 2012. Having failed to convince legislators, PAS proponents in Massachusetts hope to legalize PAS by appealing to a populace that is largely unfamiliar with the consequences in states with this deadly law on the other side of the nation. There is overwhelming scientific evidence and human experience validating the dangers of PAS, and Massachusetts voters have a responsibility to access as much of this critical information as possible before they go the polls. This includes knowledge of the text of the proposed statute which, like Oregon and Washington’s, opponents note fails to impose oversight of physicians in order to prevent abuses.
Conclusion
PAS has never been legalized when subjected to the legal and scientific scrutiny of a legislature with the ability to examine years of research that has established the damage these statutes have caused. Moreover, no studies have been completed that suggest any benefits of PAS, let alone benefits that would justify coaxing or coercing vulnerable patients to kill themselves for the benefit of others, taking the lives of those without terminal illnesses, and killing people who may have years left to live. No research exists to demonstrate that patients are benefitted by PAS. Rather, studies to date have uncovered additional negative consequences beyond those most routinely cited in opposition to this practice. Massachusetts voters should make every effort to obtain the evidence and weigh it for themselves as they go to the polls and render their judgment on Question 2 this November 6.
*See also previous CLI blog on Oregon’s 2012 Annual PAS Report.
Jacqueline Harvey, Ph.D.is a bioethicist and public policy scholar whose research primarily focuses on end-of-life legislation, particularly state policies that allow the forced removal of life-sustaining medical treatment against patient wishes. Her training includes a Ph.D. in Public Administration and an M.S. in Social Work. Dr. Harvey currently works in Texas as a policy analyst and independent evaluator, analyzing the effectiveness of government social welfare grants and human service programs for non-profit organizations.
[1] Smith, KA, Goy, ER, Havath, TA, Ganzini, L. Quality of death and dying in patients who request physician-assisted death. Journal of Palliative Medicine. 14,4. 2011.